Authors:
Paper: link
Slides/Video: link
Abstract:
Study objectives
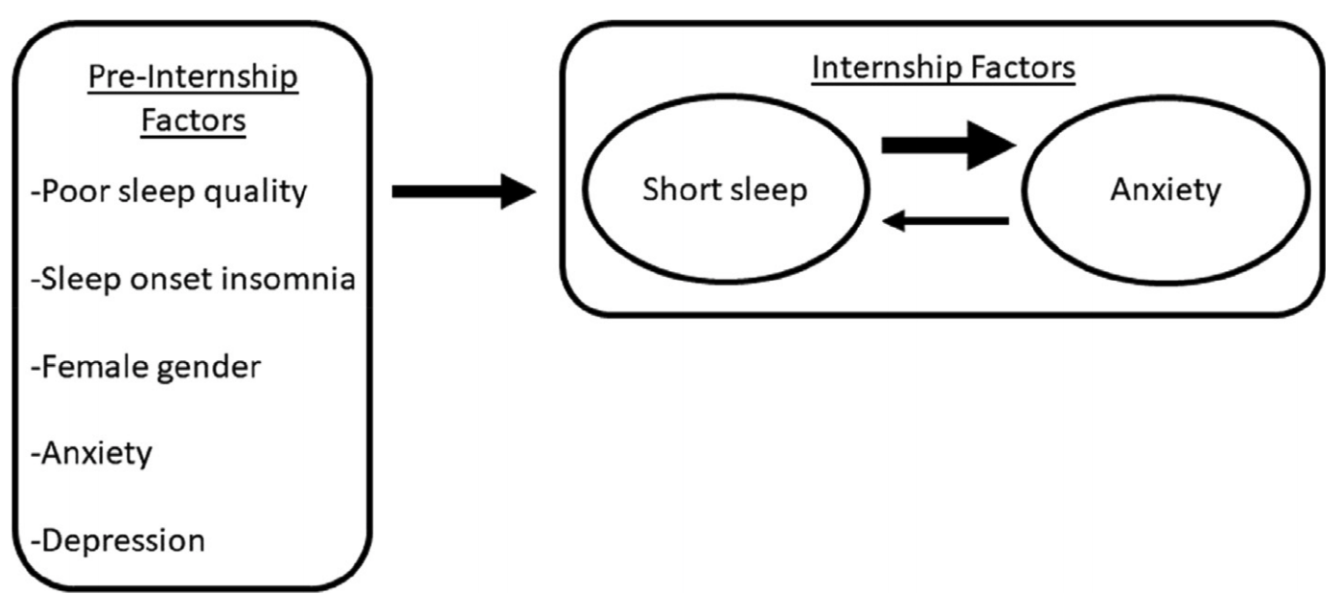
While anxiety rates are alarmingly high in short sleeping insomniacs, the relationship between insomnia and anxiety symptoms has not been extensively studied, especially in comparison to the relationship between insomnia and depressive symptoms. Using residency training as a naturalistic stress exposure, we prospectively assessed the role of sleep disturbance and duration on anxiety-risk in response to stress.
Methods
Web-based survey data from 1336 first-year training physicians (interns) prior to and then quarterly across medical internship. Using mixed effects modeling, we examined how pre-internship sleep disturbance and internship sleep duration predicted symptoms of anxiety, using an established tool for quantifying symptom severity in generalized anxiety disorder (GAD).
Results
Pre-internship poor sleepers are at more than twice the odds of having short sleep (≤6 h) during internship as good sleepers (OR = 2.38, 95% CI = 1.61, 3.57). Poor sleepers were also at twice the odds for screening positive for probable GAD diagnosis (OR = 2.08, 95% CI = 1.26, 3.45). Notably, sleep onset insomnia strongly predicted anxiety development under stress (OR = 3.55, 95% CI = 1.49, 8.45). During internship, short sleep associated with concurrent anxiety symptoms (b = −0.26, 95% CI = −0.38, −0.14) and predicted future anxiety symptoms even more strongly (b = −0.39, 95% CI = −0.76, −0.03).
Conclusions
Poor sleepers, particularly those with sleep onset insomnia symptoms, are vulnerable to short sleep and GAD anxiety and worry during chronic stress.